Abstract
INTRODUCTION
Light chain (AL) amyloidosis is a systemic disease characterized by immunoglobulin light-chain fragment deposition that predominantly affects the heart and kidneys. Cardiac involvement is the most important determinant of survival, and early diagnosis is key to improve outcome. Grogan et al. developed an electrocardiogram (ECG)-based artificial intelligence (AI) driven model that can reliably predict cardiac amyloidosis (CA) using a 12-lead ECG before clinical diagnosis, providing a tool for early detection. In this model, scores range from 0% to 100%, where score of 100% indicates the highest probability of CA.
Cardiac biomarkers, especially N-terminal pro-brain natriuretic peptide (NT-proBNP), have a strong correlation with therapeutic response and are the best predictors of prognosis. We aimed to determine if the CA ECG AI model could identify changes in amyloid probability after administration of systemic therapy in patients with amyloid cardiac involvement.
METHODS
We performed a retrospective analysis on patients diagnosed with AL amyloidosis between 2003 and 2021. Patients with cardiac involvement prior to the initiation of treatment who experienced a cardiac response following systemic therapy and had an ECG with NT-proBNP levels at baseline and after cardiac response (but before progression, if applicable) were included in the study. Only patients with ECGs within 30 days of baseline labs and with at least one ECG after achievement of cardiac response were included. Cardiac involvement, response and progression were defined based on standard criteria, as described by Comenzo et al. (Leukemia, 2012). Patients were evaluated for cardiac response using NT-proBNP at least 90 days after the initiation of treatment. Two separate analyses (cohort A and B) for response were performed using the paired two-sample t-test. For cohort A, AI-ECG CA probability at baseline was compared to AI-ECG probability from the first ECG available at first documented instance of cardiac response. For cohort B, baseline probability was compared to AI-ECG probability at the best cardiac response window, defined as the timeframe with the lowest sustained NT-proBNP levels.
RESULTS
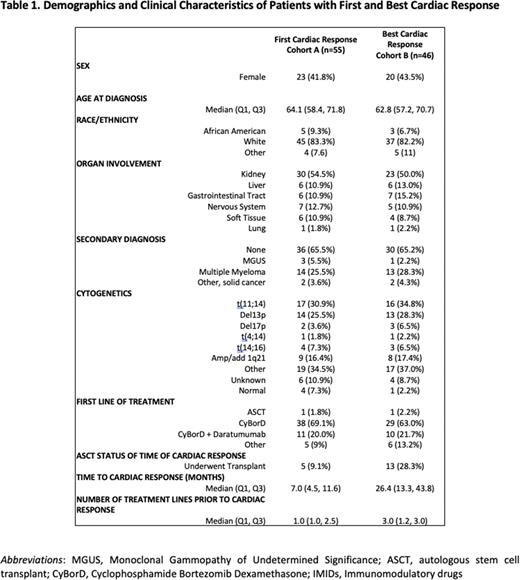
Review of electronic health records was performed on an initial cohort of 201 patients. A total of 55 and 46 patients met inclusion criteria for cohort A and cohort B, respectively. Demographics and clinical characteristics for both groups are summarized in Table 1.
Patients in cohort A had a median time to first cardiac response of 7 months, after a median of one line of treatment. Using the AI-ECG model at baseline and at first documented cardiac response, there was an 11% decrease in CA probability (85% vs. 73%, p = 0.003). Patients in cohort B had a median time to best cardiac response of 26.4 months, after a median of 3 treatment lines. There was a 21% decrease when comparing CA baseline probability to the probability at the time of best cardiac response (0.85% vs. 0.64%, p <0.001).
DISCUSSION
Using this AI ECG model, we identified a statistically significant decrease in the probability of CA after successful treatment. The AI-ECG model, a validated early diagnostic tool for CA, was able to identify post-treatment ECG changes in patients with known cardiac response. This may represent a novel cost-effective method to detect early response to therapy in CA patients. Future studies will seek to determine if CA probability is associated with extent of cardiac involvement and whether improvements in CA probability correspond to clinical outcomes and can be used to impact therapy decisions.
Disclosures
Muchtar:Protego: Consultancy; Janssen: Honoraria. Bergsagel:Oncopeptides: Consultancy; Janssen: Consultancy; GSK: Consultancy; Novartis: Consultancy; Pfizer: Consultancy. Fonseca:Oncopeptides: Consultancy; OncoTracker: Consultancy, Membership on an entity's Board of Directors or advisory committees; AbbVie: Consultancy; H3 Therapeutics: Consultancy; Caris Life Sciences: Membership on an entity's Board of Directors or advisory committees; Regeneron: Consultancy; Novartis: Consultancy; Merck: Consultancy; Amgen: Consultancy; Adaptive Biotechnologies: Membership on an entity's Board of Directors or advisory committees; Sanofi: Consultancy; Kite: Consultancy; Karyopharm: Consultancy; GSK: Consultancy; BMS/Celgene: Consultancy; Pharmacyclics: Consultancy; Pfizer: Consultancy; Juno: Consultancy; Janssen: Consultancy; Bayer: Consultancy; Takeda: Consultancy; OncoMyx: Membership on an entity's Board of Directors or advisory committees.
Author notes
Asterisk with author names denotes non-ASH members.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal